Most teams do not get tripped up by QMSR because the words are hard.
They get tripped up because they assume the change is mostly paperwork. It is not. The FDA's Quality Management System Regulation now sits much closer to ISO 13485:2016, and that changes how teams think about inspection, evidence, and control.
The real-world scenario
Picture a medtech quality team that already thinks it has a decent system.
There are approved procedures. There is a document library. There are training records. CAPA exists. Change control exists. On the surface, the quality system looks organized enough.
Then QMSR lands.
The team realizes that the real question is not whether it has documents. The question is whether the system still makes sense when FDA expectations are aligned more closely with ISO 13485 and the inspection process is no longer the one everyone used to build around.
That is where the conversation changes.
Under the old QSR, 21 CFR 820.180(c) gave internal audits, management reviews, and supplier audit reports a different treatment. Under QMSR, that old buffer is gone. Those records now sit in the inspection story.
What teams usually miss
QMSR is not just a renaming exercise.
ISO 13485 is not just a box to tick.
The change matters because it pulls the quality system closer to a shared language for:
- document control
- design and development
- complaint handling
- CAPA
- training
- supplier oversight
That means the quality system has to behave like one connected process, not a pile of records that happen to live in the same folder.
Callout: QMSR is not only about matching a standard. It is about whether the quality system still holds together when the inspection conversation changes and the record drawer is no longer off limits.
Where the old habits show up
Teams usually notice the gap in the same places:
- one procedure says one thing and the downstream records still point somewhere else
- change control exists, but the record trail feels split between tools
- supplier issues are handled, but the connection to the core quality system is thin
- review and approval happen, but the history is spread across folders and exports
- the team still treats internal review records like they are private, even though QMSR puts them in inspection scope
That is not a paperwork problem. It is a system problem.
Where it breaks in practice
| Area | Old QSR frame | QMSR / ISO 13485 shift |
|---|---|---|
| Record access | Internal audits, management reviews, and supplier audit reports often felt like support files | Those records are now part of the inspection conversation |
| Vocabulary | QSR-era files and device records could sit in separate silos | ISO 13485 pushes a more connected quality-system language |
| Risk management | Risk could feel like a downstream checkbox | Risk has to travel across the lifecycle |
| Traceability | Teams often reconstructed the story after the fact | The evidence path has to be current and defensible already |
| Inspection response | People gathered files when the ask came in | Evidence should already be organized enough to trust |
The core issue is simple. A quality system can have all the right ingredients and still feel disconnected when someone asks how the pieces fit together.
That is the glass-house shift. If your internal reviews and audit reports live like private notes, the inspection now reaches them.
Regulatory basis
FDA's QMSR page makes the change plain: the regulation became effective on February 2, 2026, incorporates ISO 13485:2016 by reference, and replaced the older QSIT inspection approach with the updated device inspection process.
That matters because medtech teams are no longer dealing with a frame that feels purely domestic. They are working in a quality system that is more aligned with international expectations and more explicit about how evidence should behave.
It also means FDA inspectors are no longer treating management review, quality audits, and supplier audit reports as records that sit outside the conversation.
This is where the glass-house feeling starts to matter. If those records were previously handled like private support files, they are now part of the inspection story.
What actually changes
- The quality system becomes easier to compare against international practice.
- Inspection expectations feel more connected to the lifecycle of the record.
- Teams need cleaner links between procedures, training, change, and follow-up.
- "We have the document" matters less than "we can still trust the record path."
- Old assumptions about what inspectors would not ask for are no longer safe.
That is also where a CSA-first mindset matters. If the evidence is current, risk-based, and easy to trace, the quality system has less to rebuild when the frame changes. Complere's validation approach fits that model because it keeps evidence current instead of forcing teams to reassemble it later.
That is the practical shift. Less comfort in the folder. More confidence in the system.
Download template
Use this checklist when you compare a current quality system with the QMSR / ISO 13485 direction:
- Can you trace a procedure change into training without searching across tools?
- Are change, CAPA, and approvals still part of one record path?
- Can QA explain the history quickly under inspection?
- Does the system make evidence easier to trust, or just easier to store?
If the answer is mostly storage, the quality system still has work to do.
Complere fit
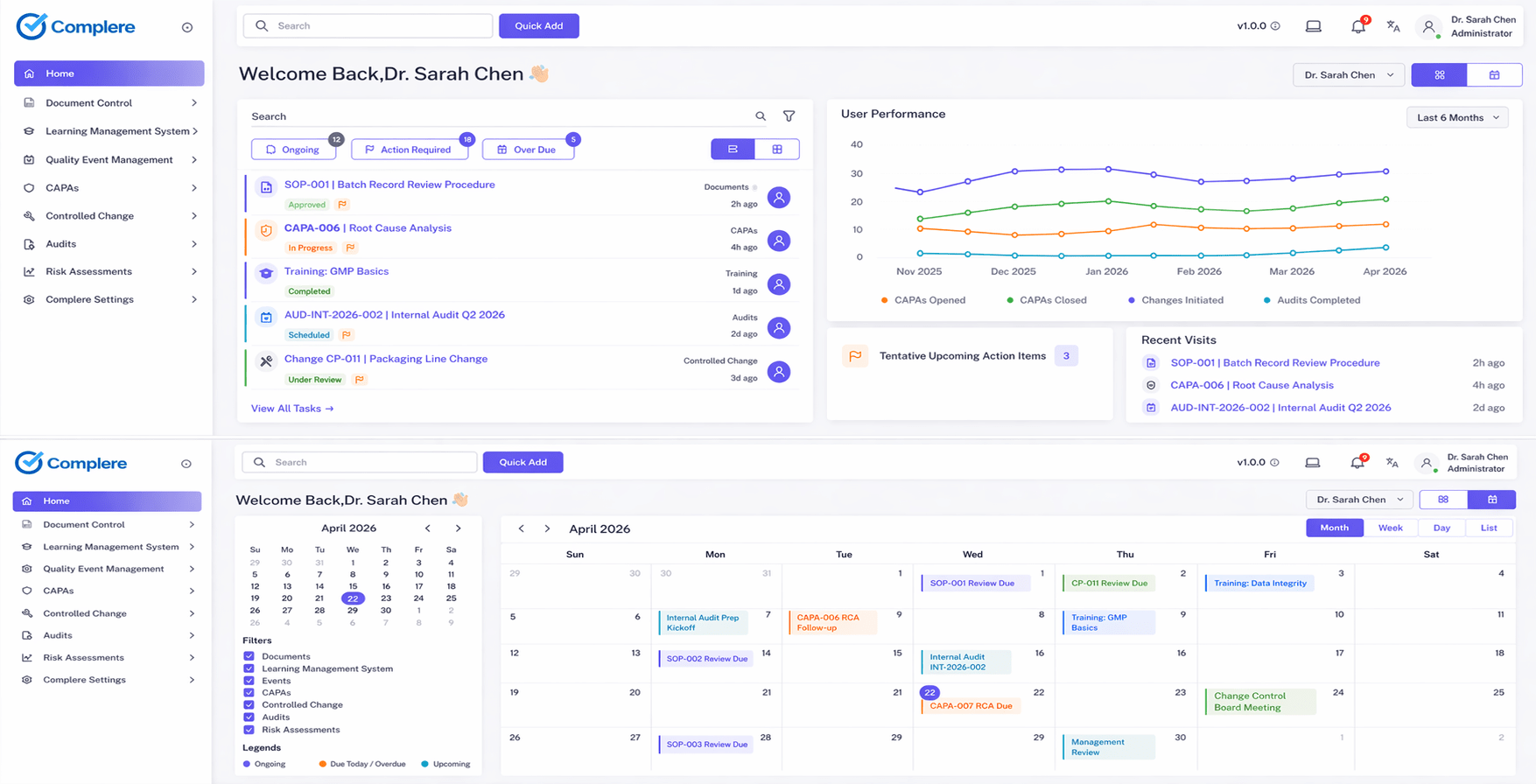
Complere fits here as a governed quality system that keeps records usable as expectations evolve.
- It supports document control, audit trails, CAPA, change control, and training in one connected workflow.
- It helps keep the evidence path current instead of forcing teams to rebuild it later.
- Its CSA-first validation model supports a current, risk-based evidence story.
- It gives teams a way to keep quality records inspection-ready without turning the system into a paperwork exercise.
That is the point for this post. Not a medtech product pitch. A practical reminder that connected records matter when the regulatory frame moves closer to the work.
This is also where most systems start to struggle. If the evidence chain is weak, the inspection just exposes it faster.
Closing thought
QMSR and ISO 13485 matter because they push quality systems toward a more connected, more inspectable way of working.
The teams that do best will not be the ones with the most files. They will be the ones with the cleanest evidence path.
Sources
- FDA Quality Management System Regulation (QMSR) page
- FDA Quality Management System Regulation Frequently Asked Questions
- FDA Overview of Device Regulation
- FDA QMSR FAQ on records previously exempt under QS regulation 820.180(c)